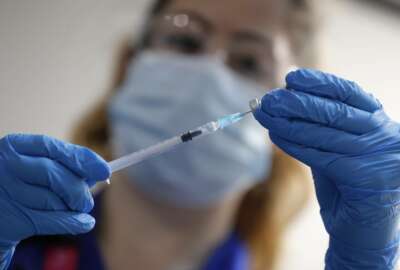
A few agencies are beginning to finalize their COVID-19 vaccination plans for federal employees.
The State Department, for example, planned to receive a limited number of COVID-19 vaccines this week, with additional shipments coming incrementally over the course of the next several months.
In an email to State employees, which Federal News Network obtained, the department said it will prioritize vaccination for the following employees:
- Frontline medical personnel,
- Personnel supporting the department’s 24/7 watch centers,
- Critical operations, maintenance and custodial staff,
- Mission critical diplomatic security personnel in the national capital region, and,
- State personnel in Kabul, Baghdad and Mogadishu “due to local conditions that can exacerbate the disease burden and the challenges of providing medical support services in these locations.”
“While we would have preferred to vaccinate our entire department workforce at once, we will have to do so incrementally based on vaccine availability,” Brian Bulatao, State’s undersecretary for management, said.
“Department leadership continues to engage with Operation Warp Speed and plans to deploy the COVID-19 vaccine to the broader workforce as soon as it is made available,” he added.
The State Department declined to confirm the details of its initial vaccination plans.
“The department’s Bureau of Medical Services’ operational medicine and logistics experts are among the best in the world at executing complex missions,” an agency spokesman said in a statement to Federal News Network. “They are planning and navigating significant distribution challenges. Due to operational sensitivity, the department is not publicly sharing specific details of the timing or logistics of the deployment of the COVID-19 vaccine for State’s workforce at this time.”
The Department of Veterans Affairs released its final COVID-19 vaccine distribution plan Tuesday, which describes the size and scope of its efforts to inoculate its workforce and veteran population.
VA began vaccinating veterans and healthcare employees on Monday. The department has 37 medical centers that are equipped to receive, handle and administer the Pfizer COVID-19 vaccine, which the Food and Drug Administration authorized last Friday.
VA ordered some 73,000 doses of the Pfizer vaccine, and those 37 facilities began receiving shipments earlier this week. A 96-year-old World War II veteran in Bedford, Massachusetts, was the first to receive the Pfzier vaccine in the VA system.
Employees and veterans at VA’s community living centers and spinal cord injury and disorder centers are at highest risk for COVID-19 and will be among the first to receive the vaccine, according to VA’s plan.
Staff at VA emergency departments, followed by COVID-19 intensive-care unit workers, non-COVID ICU employees and other staff providing face-to-face care and services for COVID-19 patients are also high-risk and eligible to receive the vaccine early on the department’s distribution efforts.
From there, VA staff working in congregate living settings and veterans in other nursing facilities without access to the vaccine would be next, followed by core hospital staff working in logistics, facilities, police operations, housekeeping, food service, occupational health and environmental engineering. A limited number of executive leadership roles could be eligible to receive the vaccine at this point as well, VA said.
“For vaccines where rate of anticipated side effects in high, it is recommended that vaccination is staggered, so that the number of personnel in each unit receiving vaccine at a given time is low,” VA’s plan reads. “This will limit absences related to response to the vaccine. Under this scenario, offering vaccine to any [healthcare professional] would be appropriate, rather than offering sequentially by risk.”
The department went on to list other healthcare workers that are part of VA’s “phase A” vaccination plan. All told, VA identified nearly 248,000 healthcare professionals.
Some 41,000 essential workers who don’t have daily, direct interactions with veterans are part of VA’s “phase B” distribution plan, as are homeless veterans, cancer patients and others.
From there, VA will vaccinate veterans based on their age. It will prioritize veterans with high-risk conditions as identified by the Centers for Disease Control and Prevention, as well as members of certain racial and ethic minority groups.
Roughly half of the 10 million veterans enrolled in VA health care are over the age of 65. Nearly 2 million African American and Hispanic veterans are enrolled with VA.
Richard Stone, VA’s acting undersecretary for health, warned Congress last week of a “long process” to vaccinate roughly 400,000 employees and 10 million veterans.
He described especially tough logistical challenges in distributing the COVID-19 vaccine to VA facilities in rural and remote locations.
The department said it will continue to update its distribution plan as more vaccines become available. FDA is currently reviewing a COVID-19 vaccine from Moderna and may approve it for widespread by the end of this week.
Stone described the Moderna vaccine as key to reaching VA’s 2 million rural veterans. The department placed an order for 122,000 doses of the Moderna vaccine, and 188 VA sites are equipped to accept it once it receives FDA approval.
Copyright
© 2024 Federal News Network. All rights reserved. This website is not intended for users located within the European Economic Area.